Benign Prostatic Hyperplasia (BPH)
Men over age 50 experience BPH symptoms
From medications to minimally invasive procedures
Most patients experience significant symptom relief
What Is Benign Prostatic Hyperplasia?
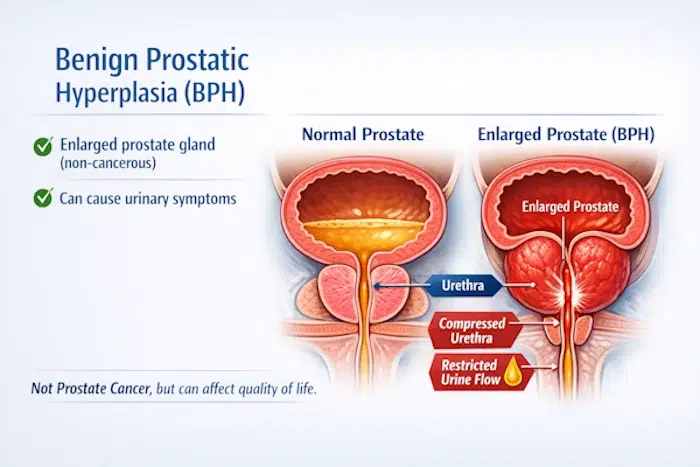
Benign Prostatic Hyperplasia (BPH) is a common condition in men as they age, characterized by the non-cancerous enlargement of the prostate gland. The prostate surrounds the urethra (the tube that carries urine out of the body), so when it enlarges, it can interfere with normal urinary function.
BPH is not prostate cancer, but it can cause bothersome symptoms that affect quality of life if left untreated.

What Causes BPH?
The exact cause of BPH is not fully understood, but it is closely linked to aging and hormonal changes—particularly shifts in testosterone and dihydrotestosterone (DHT) levels.
Risk factors include:
- Age (most common after age 50)
- Family history of prostate conditions
- Hormonal changes
- Certain lifestyle factors (obesity, inactivity)
Common Symptoms of BPH
As the prostate enlarges, it can press against the urethra and bladder, leading to urinary symptoms such as:
- Frequent urination (especially at night)
- Difficulty starting urination
- Weak urine stream
- Dribbling at the end of urination
- Feeling like the bladder isn’t fully empty
- Sudden, urgent need to urinate
These symptoms may start gradually and worsen over time.





The DTU Difference
- Expert Urologists
- Comprehensive Evaluation
- Advanced Techniques
- Personalized Care
- Discreet Environment
Frequently Asked Questions About Benign Prostatic Hyperplasia (BPH)
When should I see a doctor for BPH symptoms?
You should consult a urologist if you experience persistent urinary symptoms such as difficulty emptying your bladder, painful urination, blood in the urine, or a sudden inability to urinate (which is a medical emergency). Early evaluation can help prevent complications like bladder damage or kidney issues.
How is benign prostatic hyperplasia (BPH) diagnosed?
BPH is diagnosed through a combination of medical evaluation and testing. Your urologist may perform a symptom review and medical history, a digital rectal exam (DRE), urine testing, and a PSA (Prostate-Specific Antigen) blood test. In some cases, imaging such as ultrasound or specialized bladder function tests (uroflow studies) may also be recommended.
What are the treatment options for BPH?
Treatment for BPH depends on how severe your symptoms are and how much they affect your daily life. Options include lifestyle changes, medications, minimally invasive procedures, and surgery.
Can lifestyle changes help manage BPH?
Yes, lifestyle changes can help manage mild BPH symptoms. These may include reducing fluid intake before bedtime, limiting caffeine and alcohol, and practicing bladder training techniques to improve urinary control.
What medications are used to treat BPH?
Common medications for BPH include alpha-blockers, which relax the muscles of the prostate, and 5-alpha reductase inhibitors, which can shrink the prostate over time. In some cases, a combination of both medications may be prescribed.
What minimally invasive procedures are available for BPH?
Minimally invasive treatments include options like UroLift®, Rezūm™ water vapor therapy, and laser therapies. These procedures often provide symptom relief with shorter recovery times compared to traditional surgery.
What Our Patients Say



Take Control of Your Health
Book your private Peyronie’s Disease consultation today.







































